by Michael Robinson, University of Liverpool
The conditions of modern warfare calling large numbers of men into action, the tremendous endurance, physical and mental, required, and the widely destructive effect of modern artillery fire will undoubtedly make their influence felt in a future war, and we shall have to deal with a larger percentage of mental disease than hitherto.
A.G. Kay, ‘Insanity in the Army in Peace and War and its treatment’, Journal of the Royal Army Medical Corps, 18:2 (1912), 153.
A.G. Kay’s observation during the Russo-Japanese War, 1904-1905, challenges presumptions that military psychiatry was unknown before the outbreak of the First World War. At the time of writing, AG Kay was serving as a Lieutenant-Colonel of the Royal Army Medical Corps. Verifying Kay’s prophecy, British Army personnel ended up medically diagnosing over 80,000 men as mentally wounded during the Great War. English psychologist Charles Myers formally used the description ‘shell-shock’ for the first time in a Lancet article in February 1915. Myers had been working with a medical unit of the British Army in France, although he admitted that he did not create the label. It was already being used among troops. Myers soon recognised that ‘shell-shock’ was an ‘ill-chosen’ and ‘harmful’ label. Instead of being brought on by the explosion or shock of a shell, many serviceman exhibited mental symptoms because of the deleterious emotional and psychological impact of warfare which wore down their nerves and resilience. Indeed, some men developed mental health troubles who had not even been in active war service.

Image: Plans of Craigavon UVF Hospital for Neurasthenia and Shell-Shock. Courtesy of Public Record Office of Northern Ireland (LA/3/8/JA/12),
Belfast War Hospital
It was within the chaotic urgency of the First World War that the Belfast War Hospital was established in April 1917 to cater to mentally wounded servicemen of the First World War. Approximately 4,470 asylum beds across the United Kingdom were made available for the treatment of mentally ill servicemen in these newly established ‘War Hospitals’. The Belfast War Hospital hosted some of this contingent, although this involved displacing the entire population of the Belfast District Lunatic Asylum. There were 1,215 admissions into the Belfast War Hospital until its closure in November 1919.
There was both continuity and change in the treatment of soldier-patients. Soldier-patients were not diagnosed as insane, wore a military dress akin to physically wounded servicemen when undergoing treatment, enjoyed better recreational facilities and were provided greater liberality with regards to parole. However, the Belfast War Hospital did not provide the progressive psychotherapeutic treatment famously being offered in military hospitals at Craiglockhart and Maghull. Instead, the Belfast War Hospital relied on continuing established forms of institutional care including recreational activities complemented by rest, recuperation, and isolation. Echoing praise of the wider War Hospital network, the conduct of staff and the standard of care offered at the Belfast War Hospital was positively received by medical officials working for the British Army.

Image: Belfast District Lunatic Asylum (c. 1890-1900) which became the site of the Belfast War Hospital. Source: Public Record Office of Northern Ireland, T/418/1/86.
Shell-Shocked Veterans after the Great War
When the Belfast War Hospital closed, most mentally ill soldiers were discharged back into society. The exception here was insane veterans who required institutionalisation in public asylums. The distribution of Service Patients within Northern Irish facilities was relatively consistent throughout the inter-war period, averaging 111 patients per year. Service Patients thus constituted less than three per cent of the average national asylum population. The Ministry established the Service Patient scheme in an attempt to elevate institutionalised veterans’ insanity above the civilian insane with whom they shared facilities.
Categorised alongside private patients, with their maintenance paid for by the Ministry of Pensions, Service Patients benefited from a weekly allowance of 2/6d for ‘additional comforts’ while under treatment. Should they pass away while under treatment, they were spared burial within the asylum cemetery in a pauper’s grave with financial assistance provided to family and friends for a private burial. They were also permitted to wear distinct civilian clothing. This differentiated them from the regular asylum population and further spared them from the stigma of pauperism. However, individual conditions of institutions varied widely across inter-war Northern Ireland. This factor remained far more important in dictating the lived experience of institutional daily life rather than the status of patients.
Existing research on British veterans demonstrates how bleak post-war experiences of mentally ill veterans returning to British society were at a time when mental illness was poorly understood and highly stigmatised. My research on Ireland reveals that the experience of similarly afflicted Irish veterans was bleaker still. Four years after the Armistice, the War Office were unable to define a clear and widely-held definition of shell-shock. Neurasthenia subsequently became the primary pensionable category for mentally ill veterans. Like shell-shock, this diagnosis was incredibly broad including a variety of neuropsychiatric symptoms. By 1921, an estimated 65,000 ex-servicemen were receiving a pension for the condition in the UK with around 12,420 pensioners residing in Ireland. The Anglo-Irish War (1919-1921) and Irish Civil War (1922-1923) differentiated the Irish experience of post-war trauma from their former British comrades with veterans returning home to experience further social and political upheaval. This homecoming detrimentally impacted their recovery with medical infrastructure and welfare administration compromised by domestic turmoil.
Travel between Belfast and Dublin was potentially hazardous. The chief inspector of Artificial Limbs for veterans complained that his work assisting veterans proved dangerous in a time of widespread ambushes and shootings. One Ministry out-patient clinic in Belfast was shut for several weeks due to the volatile sectarian disturbances in the city in 1920. Mentally ill Catholic veterans in Ulster undergoing in-patient treatment in Craigavon Hospital, only one of two state-funded facilities in Ireland catering for neurasthenic veterans, suffered intimidation via anonymous personal threats. Colonel Spender, Secretary to the Cabinet, Northern Parliament believed that: ‘Probably the threats are not really of a very serious character from a purely psychological point of view, but when conveyed to ex-servicemen suffering from shell-shock, they are of a most cowardly character and unfortunately produce a great effect on the individual’. Seemingly at their own request, most Catholic in-patients were subsequently transferred to another unnamed hospital. The treatment of mentally ill Catholic in-patients at Craigavon was the very antithesis of what the Ministry’s secluded and scenic in-patient facilities were aiming to provide: complete withdrawal from the war and thoughts of conflict and danger.
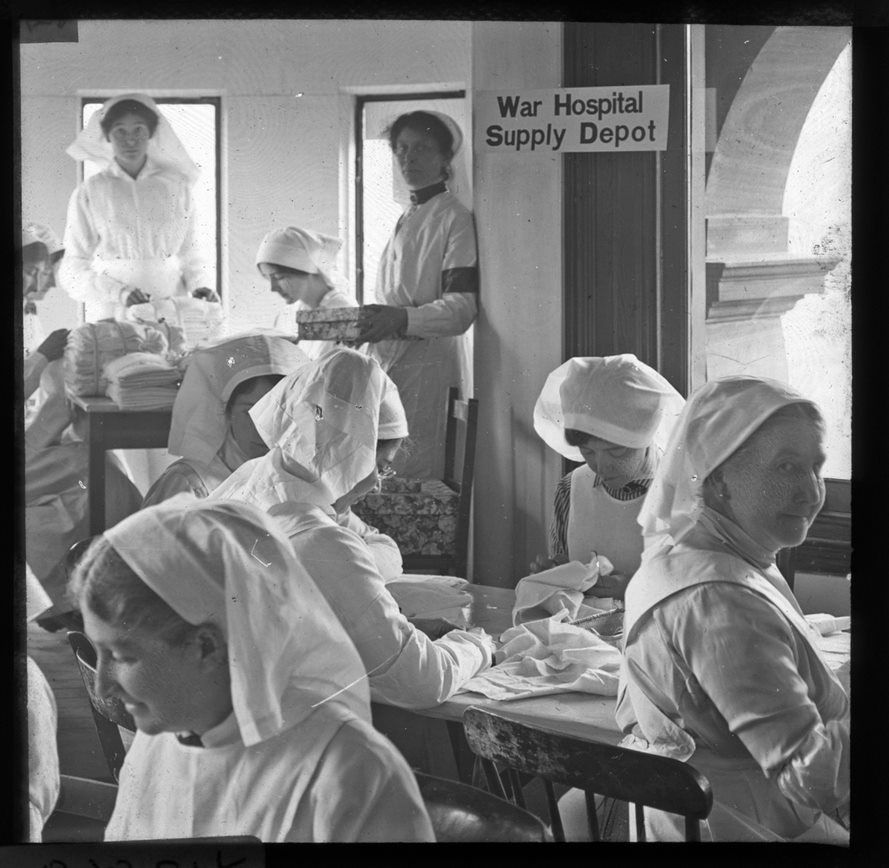
Image: First World War image of nurses in War Hospital supply depot. © National Museums NI.
After socio-political disturbances receded in the 1920s and into the 1930s, neurasthenic veterans in Northern Ireland experienced a similar homecoming to their former comrades who returned to Britain. The large majority of neurasthenic pensioners drew out their disability pensions for the remainder of their lives. The surviving files of mentally disabled veterans reveals how Craigavon Hospital continued to provide in-patient and out-patient treatment for the remainder of the inter-war period. However, whilst Armistice Day parades and poppy selling remained popular and well-observed in many communities, mentally ill veterans would suffer from retrenching government policy that sought to reduce the state’s liability towards disabled veterans. For example, British state policy mandated a seven-year time limit on disability claims in its 1921 War Pensions Act preventing mentally ill veterans from applying for a statutory pension after 1 September 1928. This policy was particularly restrictive to mental illness which can accumulate in the long-term or arise years after war service. The experiences of these veterans without the medical recognition that their mental troubles were due to war service, and who remained outside the scope of the government, remains an untold story.
In April 2020, Dr Michael Robinson published a monograph in Manchester University Press’ ‘Disability History’ series entitled: Shell-Shocked British Army Veterans in Ireland, 1918-39: A Difficult Homecoming. It was republished in paperback format on 15 February 2022.
Find out more about the book on the Manchester University Press website
© The Author(s) 2021. Published by the Epidemic Belfast team on behalf of Ulster University. Any unauthorised broadcasting, public performance, copying or re-recording will
constitute an infringement of copyright.

Where are the records of soldier patients of Belfast War Hospital held. Is it possible to access these records ?
Perhaps try PRONI, or perhaps National Archives (Kew, London)